Dr. Peter Hotez, director of the Texas Children’s Hospital Center for Vaccine Development, and Dr. Huda Zoghbi, director of the Jan and Dan Duncan Neurological Research Institute at Texas Children’s Hospital, have been elected as the newest members of the American Academy of Arts and Sciences, one of the nation’s most prestigious honorary titles.
Dr. Peter Hotez, director of the Texas Children’s Hospital Center for Vaccine Development, and Dr. Huda Zoghbi, director of the Jan and Dan Duncan Neurological Research Institute at Texas Children’s Hospital, have been elected as the newest members of the American Academy of Arts and Sciences, one of the nation’s most prestigious honorary titles.
“Membership in the Academy is not only an honor, but also an opportunity and a responsibility,” said Jonathan Fanton, president of the American Academy. “Members can be inspired and engaged by connecting with one another and through Academy projects dedicated to the common good. The intellect, creativity and commitment of the 2018 Class will enrich the work of the Academy and the world in which we live.”
The Academy is one of the country’s oldest societies and independent policy research centers. It recognizes exceptional scholars, leaders, artists and innovators and engages them in sharing knowledge and addressing challenges facing the world. This year, Hotez and Zoghbi join more than 200 other individuals from a wide range of disciplines and professions as elected members of the Class of 2018.
The Class of 2018 members were elected in 25 categories and are affiliated with 125 institutions from across the globe. They include scientists, scholars, an academy award winner, philanthropists, CEOs, historians, a past U.S. president and a current Supreme Court judge.
See a full list of new members.
The new class will be inducted at a ceremony in October 2018 in Cambridge, Mass., at which the newly elected members will sign the Book of Members, and their signatures will be added to the Academy members who came before them, including Benjamin Franklin (1781) and Alexander Hamilton (elected 1791) in the 18th century; Ralph Waldo Emerson, (1864), Maria Mitchell (1848) and Charles Darwin (1874) in the 19th; and Albert Einstein (1924), Robert Frost (1931), Margaret Mead (1948), Milton Friedman (1959) and Martin Luther King, Jr. (1966) in the 20th.
Hotez
In addition to his responsibilities at Texas Children’s, which include being the Endowed Chair in Tropical Pediatrics, Hotez is professor and dean of the National School of Tropical Medicine at Baylor College of Medicine and is a Fellow in Disease and Poverty for the James A. Baker III Institute for Public Policy at Rice University. He also holds a title of university professor at Baylor University and is founding editor in chief for the open access medical journal PLOS Neglected Tropical Diseases.
Hotez has been recognized for his work in research and advocacy as a world-renowned expert in neglected tropical diseases. He founded the National School of Tropical Medicine at Baylor College of Medicine in 2011. There, he leads an international team of scientists working to develop vaccines to combat some of the world’s most common yet potentially deadly diseases such as hookworm infection, schistosomiasis and other infectious and neglected diseases, including Chagas disease, leishmaniasis and SARS. These diseases affect millions of children and adults worldwide in some of the most poverty stricken areas.
In 2006 at the Clinton Global Initiative he helped to launch a Global Network for NTDs, and 10 years later in 2016, Hotez became known as the thought leader on the Zika epidemic in the Western Hemisphere and globally. He was among the first to predict Zika’s emergence in the U.S. He has been called upon frequently to testify before Congress and served on infectious disease task forces for two consecutive Texas governors.
Zoghbi
Zoghbi, a professor of pediatrics, molecular and human genetics, neurology and neuroscience at Baylor, is the world’s leading expert on Rett syndrome. The disease strikes after about a year of normal development and presents with developmental regression, social withdrawal, loss of hand use and compulsive hand wringing, seizures and a variety of neurobehavioral symptoms.
After encountering girls with Rett syndrome, Zoghbi set out to find the genetic cause of the disease. She and her research team identified mutations in MECP2 as the cause and revealed the importance of MeCP2 for the function of various neuronal subtypes. Her work in mouse models showed just how sensitive the brain is to the levels of MeCP2. Too little MeCP2 causes Rett syndrome; doubling MeCP2 levels causes progressive neurological deficits. The latter disorder is now recognized as MECP2 duplication syndrome.
The discovery of the Rett syndrome gene provided a straightforward diagnostic genetic test, allowing early and accurate diagnosis. It also revealed that mutations in MECP2 can cause a host of other neuropsychiatric features ranging from autism to juvenile onset schizophrenia. Further, it provided evidence that an autism spectrum disorder or an intellectual disability disorder can be genetic even if it is not inherited.
Her discovery opened up a new area of research on the role of epigenetics in neuropsychiatric disorders. Her more recent work has shown that symptoms of adult mice modeling the duplication disorder can be reversed using antisense oligonucleotides that normalize MeCP2 levels. This discovery provides a potential therapeutic strategy for the MECP2 duplication syndrome and inspires similar studies for other duplication disorders.
Zoghbi and collaborators also have made many discoveries toward understanding mechanisms driving adult-onset neurodegenerative disorders and are now focused on identifying potential therapeutics for these disorders.
















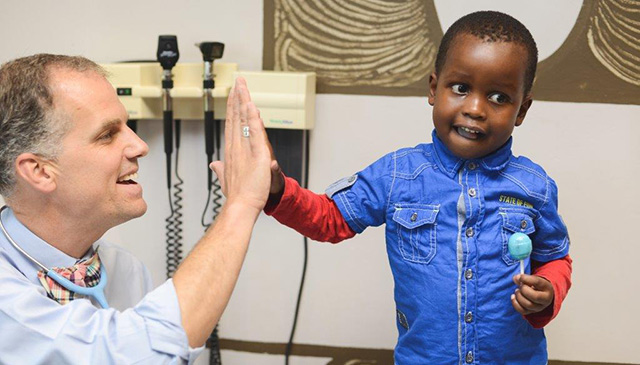 Just 12 short months ago, Texas Children’s Cancer and Hematology Centers, Baylor College of Medicine International Pediatric AIDS Initiative at Texas Children’s Hospital, the Bristol-Myers Squibb Foundation, and leaders in Botswana, Uganda and Malawi, announced a $100 million initiative to create an innovative pediatric hematology-oncology treatment network in sub-Saharan Africa.
Just 12 short months ago, Texas Children’s Cancer and Hematology Centers, Baylor College of Medicine International Pediatric AIDS Initiative at Texas Children’s Hospital, the Bristol-Myers Squibb Foundation, and leaders in Botswana, Uganda and Malawi, announced a $100 million initiative to create an innovative pediatric hematology-oncology treatment network in sub-Saharan Africa. Dr. Peter Hotez, director of the Texas Children’s Hospital Center for Vaccine Development, and Dr. Huda Zoghbi, director of the Jan and Dan Duncan Neurological Research Institute at Texas Children’s Hospital, have been elected as the newest members of the American Academy of Arts and Sciences, one of the nation’s most prestigious honorary titles.
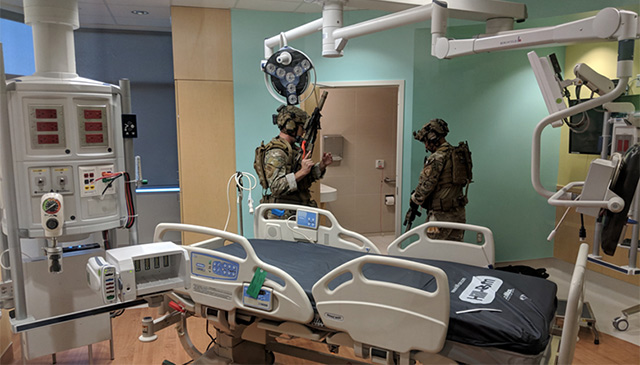
Dr. Peter Hotez, director of the Texas Children’s Hospital Center for Vaccine Development, and Dr. Huda Zoghbi, director of the Jan and Dan Duncan Neurological Research Institute at Texas Children’s Hospital, have been elected as the newest members of the American Academy of Arts and Sciences, one of the nation’s most prestigious honorary titles. Texas Children’s Hospital’s Trauma Center has received the prestigious 2018 Trauma System of Care Award from the Southeast Texas Regional Advisory Council (SETRAC). The Trauma System of Care Award recognizes Texas Children’s Hospital as one of the best in SETRAC’s nine-county region for excellence in the development and advancement of pediatric trauma services.
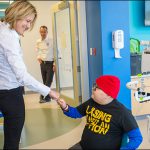
Texas Children’s Hospital’s Trauma Center has received the prestigious 2018 Trauma System of Care Award from the Southeast Texas Regional Advisory Council (SETRAC). The Trauma System of Care Award recognizes Texas Children’s Hospital as one of the best in SETRAC’s nine-county region for excellence in the development and advancement of pediatric trauma services. On April 18, Olympian Kristin Armstrong and Scott Schnitzspahn, vice president of Elite Athletics, USA Cycling, met with employees and visited with patients during a tour of Texas Children’s Hospital The Woodlands. Armstrong, a three-time gold medalist, and Schnitzspahn brought smiles to many of the patient’s faces and were enjoyed by the many employees and leaders who got to meet them.
On April 18, Olympian Kristin Armstrong and Scott Schnitzspahn, vice president of Elite Athletics, USA Cycling, met with employees and visited with patients during a tour of Texas Children’s Hospital The Woodlands. Armstrong, a three-time gold medalist, and Schnitzspahn brought smiles to many of the patient’s faces and were enjoyed by the many employees and leaders who got to meet them.