
More than 400 employees and staff with 7,460 combined years of Texas Children’s service and expertise were given the royal treatment last week at the organization’s 27th Annual Employee Recognition Celebration.
Held on May 19 at the Bayou Event Center, the honorees dined at tables wrapped in linens and adorned with glittering candles and plush red, white and green flowers. After lunch, each honoree was led down a red carpet and onto a stage where President and CEO Mark A. Wallace and others shook their hands and thanked them for their 15, 20, 25, 30 and 40 years of service to Texas Children’s.
In addition to long-time honorees, recipients of the Best of the West, Mark A. Wallace Catalyst Leadership, Smiles and Super Star awards were recognized.
“You are the face of Texas Children’s Hospital. It’s not me, it’s not Dr. Andropoulos, it’s not Dr. Fraser, it’s not Dr. Kline,” Wallace said to the crowd. “It’s our 10,000 employees because you are here 24/7 every day.”
Valesca Adams, one of 10 honored for their 40-year milestone anniversary with Texas Children’s, said the organization and her job in Renal and Pheresis Services are a huge part of her life. In addition to “really liking” the people she works with, Adams said she loves the children and families she comes into contact with daily at the hospital.
“I love my job,” she said. “It’s fun to get up and come to work every day.”
Senior Vice President Linda Aldred said the annual employee recognition ceremony is a time to honor those who have given so much to carrying out the values and the mission of Texas Children’s to provide unparalleled family-centered care for our patients and their families.
“When people love what they do, when they believe in what they are doing, the results can be staggering and the contribution is too big to count,” Aldred said. “Your dedication is the heart of Texas Children’s past, present and future greatness, and that’s exactly what we are here to celebrate today.”
Congratulations to all of the honorees!
A copy of the event’s program can be found here.





































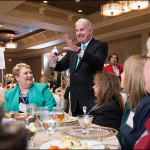




 “The OCT is an imaging tool that is similar to ultrasound but uses light waves instead of sound waves to create high resolution images of the retina and optic nerve,” said pediatric neuro-ophthalmologist Dr. Veeral Shah. “This type of imaging allows us to detect changes in retina and optic nerve structure that may reflect loss and damage of visual function that might not be visible with an ocular examination.”
“The OCT is an imaging tool that is similar to ultrasound but uses light waves instead of sound waves to create high resolution images of the retina and optic nerve,” said pediatric neuro-ophthalmologist Dr. Veeral Shah. “This type of imaging allows us to detect changes in retina and optic nerve structure that may reflect loss and damage of visual function that might not be visible with an ocular examination.”


