July 21, 2015
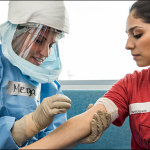
 Two nurses and a doctor donned personal protective equipment before entering the hospital room to check on the young patient who was exhibiting signs of a highly infectious disease.
Two nurses and a doctor donned personal protective equipment before entering the hospital room to check on the young patient who was exhibiting signs of a highly infectious disease.
While the physician patiently talked with the child’s worried mother, the nurses checked the patient’s vitals and drew a blood sample to be tested for diseases such as Ebola, Lassa and Marburg fevers.
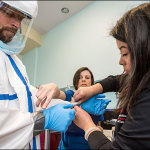
A lab technician dressed in personal protective equipment gathered the blood sample and took it to a nearby lab that would produce results within hours.
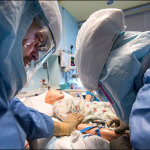
Meanwhile, the doctor and nurses worked with a team of medical professionals watching and advising from an adjacent room equipped with an observation window to keep the patient stabilized.
Fortunately, this was not a real scene at Texas Children’s Hospital West Campus but a detailed simulation that recently occurred in the soon-to-be-finished special isolation unit.
In October, the state-of-the-art facility will open its doors and a Special Response Team will stand ready to receive children suspected of having a highly contagious disease.
“Having a special isolation unit at Texas Children’s Hospital West Campus will allow our system to offer our exemplary medical care to a very vulnerable population,” said West Campus President Chanda Cashen Chacón. “We have made tremendous progress since announcing the project in December and are still working full speed ahead.”
Construction on the eight-bed unit is near completion with operational planning, team training and final construction progressing rapidly. The project is like no other at Texas Children’s since the special isolation unit will incorporate all of the latest scientific and technological approaches to biocontainment, including negative air pressure, laminar air flow, high-efficiency particulate air (HEPA) filtration, separate ventilation, anterooms, biosafety cabinets, a specialized laboratory, special security access and autoclaves.
When complete, the unit will be fully equipped to care for any infant or child with a serious communicable disease, with all of the measures available to assure safety of the health care team, other patients and their families. The specialized biosafety level 3 laboratory will enable the care team to monitor the progress of patients and perform rapid detection methods to identify unusual pathogens.
Dr. Gordon Schutze will serve as medical director of the special isolation unit and Drs. Judith Campbell and Amy Arrington will be the unit’s associate medical directors. An elite volunteer-based team of experienced nurses and physicians – all of whom will have successfully completed an intensive advanced certification course and practicum in infection control, hospital epidemiology and management of infectious diseases in the critical care setting – will staff the unit.
Many members of the Special Response Team have been chosen, however recruitment for physicians, nurses, laboratory technicians and environmental services personnel is ongoing. To learn more about joining the Special Response Team, click here.
“The team that staffs this unit is key to making it successful,” Campbell said. “Many of our talented staff have stepped up to the plate to participate in this noble endeavor and we need more to raise their hands to volunteer.”
Another aspect of the unit that has recently ramped up is training and education. Led by Arrington, the training and education program for the special isolation unit is robust and has already included two almost full-day simulations. The first of which was a mid-construction simulation to assess any environmental issues important to the performance, health, comfort and safety of both our patients and our medical staff. The second simulation focused on clinical scenarios involving a patient suspected of having a highly contagious disease.
“The more we train the better off we will be in the event of an infected patient,” Arrington said. “It’s an ongoing process.”
 Have you ever wondered what it feels like to run on the floor of NRG Stadium, home of the Houston Texans? If so, you and your child now have a chance. All you have to do is sign up for the TORO’S Kids 1K on Sunday, September 20.
Have you ever wondered what it feels like to run on the floor of NRG Stadium, home of the Houston Texans? If so, you and your child now have a chance. All you have to do is sign up for the TORO’S Kids 1K on Sunday, September 20.