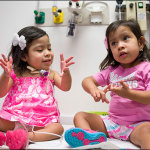
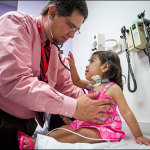
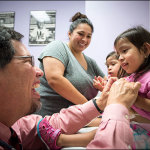
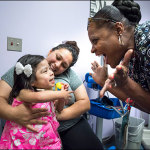For non-English speaking families like Argelia Diaz, she knows that when she comes to Texas Children’s, she can always count on a Spanish-speaking interpreter to help her communicate with her daughter’s medical team.
For non-English speaking families like Argelia Diaz, she knows that when she comes to Texas Children’s, she can always count on a Spanish-speaking interpreter to help her communicate with her daughter’s medical team.
“I don’t know what I would do without them,” Diaz said through her interpreter. “They give us all the information that the providers want to tell us and help break down the medical terms for us. They are very kind and are always there whenever we need them.”
As an internationally recognized referral center, Texas Children’s cares for many international patients including those here at home who do not speak English. These patient families rely solely on the skills and expertise of Texas Children’s Language Services Department to bridge the communication barrier.
“Language barriers have the potential to adversely impact patient care and outcomes,” said Language Services Manager Alma Sanchez. “Issues like misdiagnosis, lack of compliance, medical errors and readmissions can all be further compounded when a patient has limited English proficiency. Communicating with them in their preferred language ensures everyone is on the same page regarding the care and treatment of the patient.”
Being an interpreter at Texas Children’s is more than just speaking a foreign language fluently. As the primary liaison between the physician and patient, interpreters ensure accurate and seamless communication is delivered to both parties during every phase of the health care process. Specially trained in diverse areas including medical terminology, modes and standards of interpretation, standards of ethics and intercultural communication, interpreters also serve as a cultural broker in the communication of information since there are many factors that may impede a patient or family’s clear understanding of a medical diagnosis or treatment plan.
“While speaking in the family’s native language, we explain their child’s diagnosis and ensure they understand all of the instructions provided by their care team,” said Violeta Riccio, project analyst at Language Services. “We also help the providers understand the patient’s concerns or questions in order to resolve any potential issues.”
On average, the Language Services Department receives 12,000 language requests per month – 4,000 are in-person interpretations, 7,000 are telephonic and 1,000 are through a mobile video system called My Accessible Real Time Trusted Interpreter (MARTTI) where an external interpreter can be contacted via live video. These capabilities enable Texas Children’s to provide interpretations in about 170 different languages.
To meet the growing demand for this service, Texas Children’s has 28 interpreters dispersed across several campuses – 17 at Texas Children’s Main Campus, five at Texas Children’s Hospital West Campus, four at Texas Children’s Pavilion for Women and two interpreters at Texas Children’s Hospital The Woodlands. Spanish is the most requested language for interpretation followed by Arabic, Vietnamese and Chinese-Mandarin.
Just like our patient families, Texas Children’s health care teams benefit greatly from this service too.
“Having an interpreter physically present is crucial to effective communication particularly in stressful situations when children are undergoing procedures or when critical information is being conveyed,” said Dr. Larry Hollier, chief of plastic surgery at Texas Children’s. “Having an onsite interpreter in the ambulatory surgery area has been transformative in terms of family satisfaction and the efficient and safe flow of children through the area.”
To learn more about Language Services, drop by their office located on the third floor of West Tower across from the gift shop. Click here to watch a video spotlighting a day in the life of interpreters at Texas Children’s.
 Texas Children’s is the honored sponsor for every Tuesday’s “Houston Legends” series. We will showcase the legendary care Texas Children’s has provided since 1954, and focus on milestone moments in our unique history. Also, a complementary website offers a more detailed look at our past, our story and our breakthroughs.
Texas Children’s is the honored sponsor for every Tuesday’s “Houston Legends” series. We will showcase the legendary care Texas Children’s has provided since 1954, and focus on milestone moments in our unique history. Also, a complementary website offers a more detailed look at our past, our story and our breakthroughs.