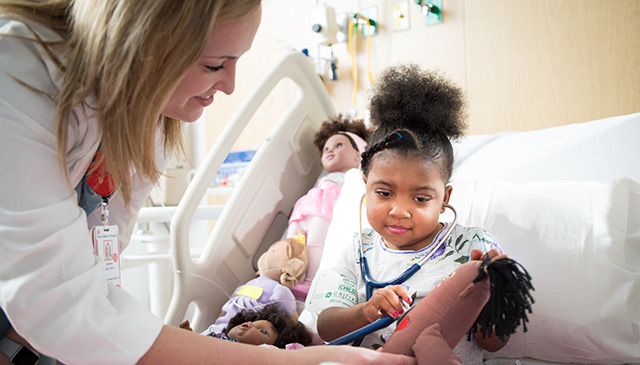February 12, 2019

When nothing seems to calm 4-month-old Bella Deborbieris, her family and caretakers in the Neonatal Intensive Care Unit know who to call – Texas Children’s Music Therapist Alix Brickley.
Within minutes of Brickley’s arrival to the side of Bella’s crib, a sense of peace and joy washes over the infant, whose big blue eyes stay focused on the music therapist while she strums her half-size guitar and softly sings the theme song to the Disney movie Frozen.
“Alix and her music work every time,” said Bella’s aunt, Kerry Kernwein. “It’s a relief knowing she’s here.”
Brickley is a member of Texas Children’s Child Life Department’s newly formed Creative and Therapeutic Arts Program. The program is comprised of four music therapists, one art therapist and a media producer, all of whom work collaboratively to alleviate stress and anxiety, while promoting positive coping skills, for patients and families during their time at Texas Children’s.
“With more than 50 child life professionals, Texas Children’s has one of the best child life departments in the country,” said Maggie Lampe, assistant director of Clinical Support Services. “This new program will enrich and support the services we already offer to support children and families as they adjust to the hospital experience.”
Each therapist is assigned a caseload throughout our Texas Medical Center Campus, working with many of their patients daily. Art Therapist Ashley Wood spent a lot of time with 12-year-old Tyrese Neal throughout his lengthy stay at Texas Children’s Heart Center. She and the heart transplant patient created masks that represented how he was feeling at the time. They also used colorful thread to make worry dolls.
“The movement used to create the dolls is very therapeutic,” Wood said. “It’s something patients can do to cope with all of the emotions they are dealing with during their stay and after they return home.”
The role of Child Life Media Producer Ashby Gleditsch on the new team is to work with the therapists to produce interactive programming for Texas Children’s Hospital’s closed circuit television station Z-TV, which can be viewed on channel 19 of any cable-connected television in the hospital.
Some of that programming – music concerts – is prerecorded and other shows – Bailey Bingo – are live. Gleditsch also works with the therapists on the team to create videos for specific patients. All of her projects, she said, are aimed at enhancing a patient’s self-concept and leaving them with a good impression of Texas Children’s.
“Giving our patients an outlet to creatively express their emotions is really powerful,” Gleditsch said.
The other members of the Creative and Therapeutic Arts Program are Marial Biard, Abi Carlton and Michael Way, all of whom are music therapists. Day in and day out they garner smiles, giggles and outright laughter from patients and family members with the magic they make via their guitars, drums, voices and other instruments, some of which are half size so they can bring them into tight spaces such as the NICU and so they can play softly as to not disturb patients who might be sleeping.
Carlton said she spends a lot of time with patients who are sedated and often intubated, and that she adjusts the music she makes to match their vital signs, and then slowly changes it to guide her patients to a more comfortable state with decreased agitation and perception of pain.
“Music may be the only positive form of stimulation these patients are able to perceive at times, and it can have powerful outcomes,” Carlton said. “Music therapy can also create positive memories and provide a sense of calm in the room that families and even staff can benefit from. It’s a real privilege to work alongside the care team with these critical care patients and see how music therapy can be such an effective modality.”
Way, a Renal Services music therapist and a member of the new Creative and Therapeutic Arts Program, works with nephrology patients across the hospital. Through music, he’s able to help patients through the many burdens of kidney disease.
“Kidney disease affects many different aspects of a patient’s life,” Way said. The burden can be staggering. I try to help patients express some of their struggles and frustrations through music.”
Biard said she loves being a music therapist at Texas Children’s because she gets to be the highlight of her patients’ and families’ days.
“We are part of their stay and they associate us with happiness,” she said. “We achieve this through music by creating everlasting memories in the recording studio, relieving their pain with song, making their bodies stronger with instrument play, and helping them express emotions in a positive way.”
Learn more about Texas Children’s Child Life Department at https://www.texaschildrens.org/departments/child-life.