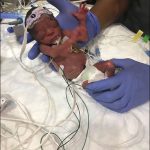
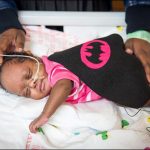
COVID-19 has affected much of what we do here at Texas Children’s but there are still areas of our system where things are almost, well, normal. One of those areas is the Labor and Delivery Unit at the Pavilion for Women where new babies are born every day and families celebrate some of the best moments of their lives.
“No one is canceling having a baby,” said Lynda Tyer-Viola, vice president of nursing at the Pavilion for Women. “The deliveries are still coming and we are going the extra mile to help our patients make joyful, lifelong memories despite what’s going on outside the walls of their hospital rooms.”
These efforts combined with precautions and protocols established to minimize any potential exposure to COVID-19 are helping ease the anxiety of expectant mothers who are having babies during this historic and unprecedented time.
To protect patients and families from the potential spread of COVID-19, members of the Labor and Delivery team are wearing masks in patient-facing settings, screening patients and visitors for symptoms of the disease, and limiting the number of visitors who come into the unit to see their loved one. Other than that, things are pretty much business as usual.
“All of the changes we have made have been embraced by both patients and families, and staff, Tyer-Viola said. “Everyone has been extremely supportive and seems to understand that we are doing what is best for everyone involved.”
Kristin Thorp, assistant clinical director of nursing at the Pavilion for Women, agreed and said she is extremely proud of her team for being so adaptive during this event and for always keeping their attention and focus on what matters most – our patients.
“Team members have exhibited a lot of grace and have been extremely nimble during this entire process,” Thorp said. “They have really stepped up to care for our patients and themselves during this unique time in history.”
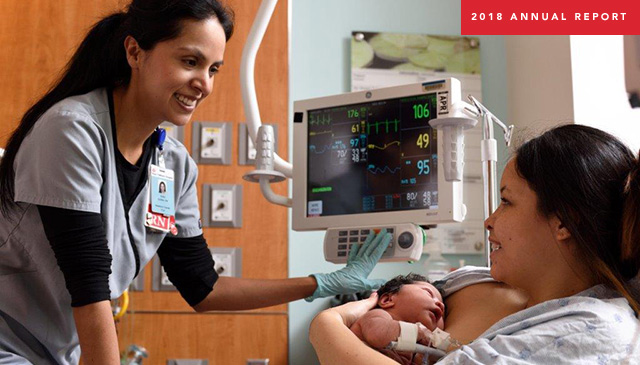
Natalia Angulo Hinkson, a new mom and a Texas Children’s employee, delivered her first child, Isabel Iris, on March 27 at the Pavilion for Women. Prior to the outbreak of COVID-19, Hinkson said she had talked to several colleagues and friends about what to expect from the experience and had made plans accordingly.
Post-delivery, she said outside of the precautions made to protect her and her daughter, and a few tweaks in her own plans to align with those measures, everything went like she hoped it would. Her husband was able to be in the delivery room with her when Isabel was born, her doctor was there to deliver the 6 pound 6 ounce bundle of joy, and her labor and delivery nurses and support staff were cool, calm, reassuring, warm and friendly.
The biggest change Hinkson said she had to make and accept was that her extended family was not able to be at the hospital during delivery. She said she had planned for them to be in the lounge and for her mom to come into the delivery room if there were complications. Fortunately, there were not, and her family is standing by to meet Isabel when it’s safe for all parties involved.
“There were things that were different and not possible, but it felt like everything my friends had told me about,” Hinkson said. “Any apprehension I had went away once I was at the hospital under the team’s care. They were extremely professional, prepared and attentive to making my experience the best it could be during what is obviously a very unusual time.”
Tyer-Viola said her team and the hospital as a whole have weathered many storms and that we’ve always ended up stronger and better than before.
“This pandemic will be no different,” she said. “We are resilient and we are dedicated wholeheartedly to our mission of caring for children and women.”
Texas Children’s Public Relations and Social Media teams are looking to share stories such as these on social media. If you delivered your baby at the Pavilion for Women during the COVID-19 pandemic, we’d love to hear your story to potentially be featured on the Pavilion for Women’s Facebook page. Please contact vxjavor@texaschildrens.org with your story.