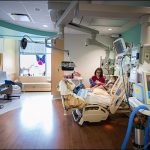
Ten-year-old Skye Jeary couldn’t believe her eyes as she was wheeled into her new, spacious room in Texas Children’s Legacy Tower. She was in awe when she saw the size of her room and commented on how she’ll have plenty of space to accommodate her stuffed unicorn and her mom who is in a wheelchair.
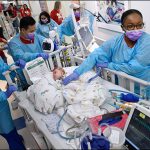
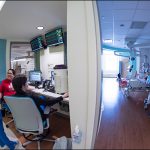
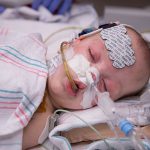
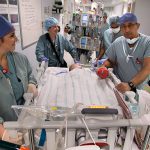
On May 22, Texas Children’s reached an historic milestone when the doors of Legacy Tower opened for the first time to care for our most critically ill patients. Beginning at 7 a.m., seven specially trained clinical teams began safely transporting 45 critically ill patients from the pediatric intensive care unit and progressive care unit in West Tower to their new, spacious, state-of-the-art critical care rooms in Legacy Tower.
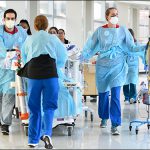
More than 150 Texas Children’s staff members were involved in the patient move to Legacy Tower, and the careful transfer of the patients took seven hours, which was a lot sooner than originally anticipated due to the efficiency and effectiveness of the Legacy Tower teams involved on Move Day.
“The planning for the patient move was unbelievably detailed,” said Dr. Lara Shekerdemian, service chief of Critical Care Services at Texas Children’s. “The patient move involved nursing, administration, physicians, nurse practitioners, all members of the team as well as the amazing family support team that guided the families through what could have been a potentially overwhelming event for them.”
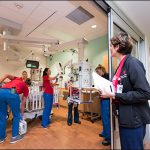
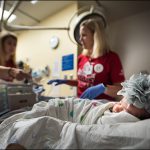
Patient and family services teams were assigned to each family member to help accompany and escort them from their current unit to the new unit in Legacy Tower and to get them settled in their new rooms.
“Our families were so excited about the move,” said Michelle Lawson, director of Texas Children’s Clinical Support Services. “They were being cheered on along the way and they were excited to be in their brand new space. They couldn’t believe we built it just for them.”
The Legacy Tower Go Live Support Center was set up on the fourth floor of Texas Children’s Pavilion for Women and comprised of 867 individuals from across the hospital system who focused on patient move tracking from West Tower to Legacy Tower. The team included support staff from Supply Chain, Security, BioMedical Engineering, Facilities Operations, Information Services, Pharmacy, Respiratory Care, as well as ancillary support teams from Texas Children’s Hospital The Woodlands, Texas Children’s Hospital West Campus and our Health Centers.
“We had floor plans on the wall that were physically tracking the patients as they moved from West Tower to Legacy Tower,” said Matt Timmons, director of Business Operations and Support Services at West Campus. “We also documented it on a spreadsheet displayed on projectors so anybody in the Go Live Support Center knew exactly where our patients were throughout the entire move process.”
While patients were being moved safely to Legacy Tower, Mission Control ensured a smooth process for the patient move by collaborating with teams from the The Woodlands Campus and West Campus to manage the inflow of patients across the system while the move process was underway.
Seven hours after the patient move process began, staff cheered and clapped their hands as the last patient was moved to Legacy Tower.
“We call today the Super Bowl of patient moves,” said Texas Children’s Vice President of Nursing Gail Parazynski. “We observed the tireless leadership, unity, and undying compassion our team has exhibited all week during the first phase of the Legacy Tower Go-Live. The success of this go-live is a true testament to the leadership and dedicated teamwork at Texas Children’s Hospital.”
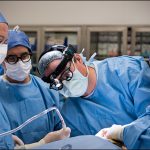
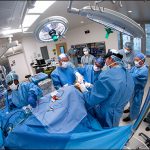
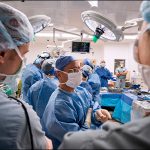
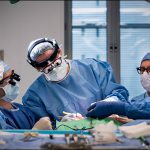
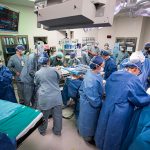
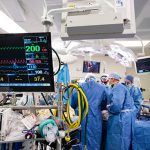
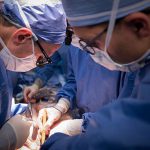
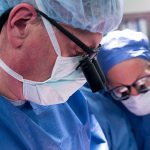
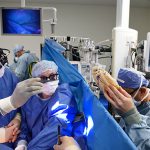
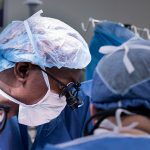
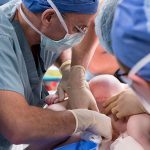
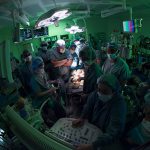
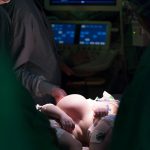
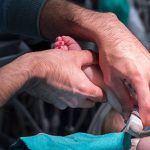
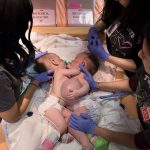
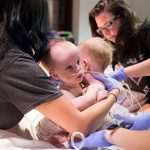
One day after this historic move, the first surgery was successfully performed in the new state-of-the-art operating room in Legacy Tower.
View the photo gallery of the patient move to Legacy Tower below. Click here to read the story of the first surgery in Legacy Tower and watch video of the state-of-the-art features of our new OR in Legacy Tower.
The second phase of Legacy Tower will open in September and house Texas Children’s Heart Center®, ranked No. 1 in the nation by U.S. News & World Report for cardiology and heart surgery.















































 Texas Children’s Hospital is committed to creating the best possible experience for our patients and their families. A significant part of this experience, that perhaps at times goes unnoticed, is our linen services. Linen forms an integral part of the services we provide – from clinical visits, to emergency visits or long stays.
Texas Children’s Hospital is committed to creating the best possible experience for our patients and their families. A significant part of this experience, that perhaps at times goes unnoticed, is our linen services. Linen forms an integral part of the services we provide – from clinical visits, to emergency visits or long stays.







 Texas Children’s Pediatrics acquired its first practice site in 1995. Two decades later, 50 more have been added and as of December 2017, all practices, hold the highest Patient Centered Medical Home (PCMH) recognition from the National Committee for Quality Assurance (NCQA).
Texas Children’s Pediatrics acquired its first practice site in 1995. Two decades later, 50 more have been added and as of December 2017, all practices, hold the highest Patient Centered Medical Home (PCMH) recognition from the National Committee for Quality Assurance (NCQA). A lot happens behind the scenes before patients are wheeled into the operating room at Texas Children’s Hospital to undergo surgery. Technicians disinfect the OR from top to bottom and a team of people with the Sterile Processing Department clean, prepare, assemble and sterilize surgical instruments for patient care.
A lot happens behind the scenes before patients are wheeled into the operating room at Texas Children’s Hospital to undergo surgery. Technicians disinfect the OR from top to bottom and a team of people with the Sterile Processing Department clean, prepare, assemble and sterilize surgical instruments for patient care. A little over a year ago, Texas Children’s Hospital The Woodlands Outpatient Building opened its doors to the Greater Houston area and beyond. Since then, the ever-growing team of providers and support staff have seen 50,000 plus patients in the outpatient areas and received numerous compliments from the patients and family members they serve.
A little over a year ago, Texas Children’s Hospital The Woodlands Outpatient Building opened its doors to the Greater Houston area and beyond. Since then, the ever-growing team of providers and support staff have seen 50,000 plus patients in the outpatient areas and received numerous compliments from the patients and family members they serve.