Last week, years of planning and hard work culminated in a special ribbon cutting ceremony and open house for employees to celebrate the grand opening of Texas Children’s Hospital North Austin. With the opening of North Austin Campus, we expand our hospital reach to four campuses, three of which are located in the Greater Houston area, including the esteemed Texas Medical Center.
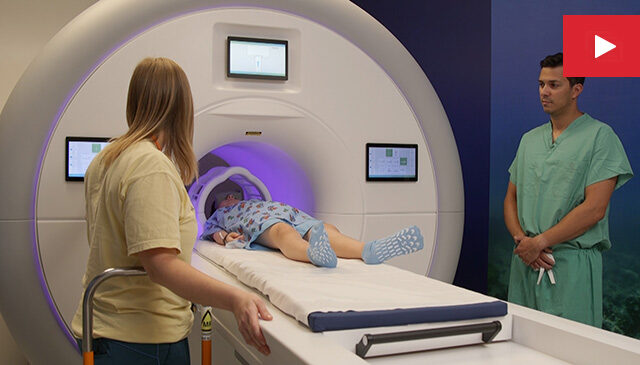
The ribbon cutting just so happened to take place on Texas Children’s platinum anniversary, and with a “1-2-3, cut the ribbon!” we signaled a major milestone in our 70-year history. Afterwards, local press, community leaders, friends and partners of Texas Children’s were invited to take a first look at the $485 million, state-of-the-art, 365,000-square-foot campus through guided tours – exploring different areas of the hospital and taking in its unique design inspired by Central Texas landscape and ecology.
This changes everything in Austin
In the last 10 years, an estimated 30,000 children had to leave Austin and travel to Houston to receive specialized care. “Austin families and the surrounding communities deserve the most advanced treatment from world-renowned physicians at any given moment,” said Austin Senior Vice President Russ Williams. “Texas Children’s is doing their best to ensure this will happen now and in the future.”
Texas Children’s has been building a presence in Austin since 2018 with more than 20 locations offering pediatric, women’s, urgent and specialty care in the region. The opening of North Austin Campus – starting with outpatient clinics on Feb. 5 and inpatient services on Feb. 20 – will provide Austin families and surrounding communities with access to top-ranked services closer to home. What’s inside North Austin Campus? Here is just a highlight:
- Five floors with 52 patient beds
- 13-room emergency center seeking Level II designation
- 11 urgent care rooms
- 12-room NICU seeking Level IV designation (the highest level)
- 10 ICU beds with room for another 14
- Seven operating rooms (five for pediatrics and two for women’s)
- Dedicated rooms for full L&D, recovery and postpartum stays
- Renal/dialysis unit
- Sleep study and epilepsy monitoring rooms
- 170,000-square-foot outpatient building with a Texas Children’s Pediatrics clinic
“It has been a longtime goal of mine to continue the incredible mission of our founders and expand access to Texas Children’s high-quality level of care to families throughout Texas,” said CEO Mark A. Wallace. “As we celebrate our 70th anniversary as an organization, we are looking forward to serving even more children and women with one of the most elite clinical teams in the world.”
The right people make the difference
Opening a brand new hospital would not be possible without the passion and dedication of our One Amazing Team, including hundreds of newly hired employees and 75+ staff transfers who bring over 600 years of Texas Children’s experience to Austin.
After cutting the ribbon, we rolled out the red carpet for these team members and their families for an Employee Extravaganza complete with swag bags, food and beverage trucks, Terry Black’s BBQ, face painting, photo stations, live music and so much more. It was an evening to remember as more than 2,000 people filled the halls of North Austin Campus to marvel at the space and enjoy the festivities.
“It was a really fun and thoughtful event,” said North Austin social worker Claire Andrefsky. “It was nice to be able to show my family the hospital, especially because it’s been such a busy year leading up to opening.”
“I am most excited about all our services being in one place, it makes my job to help families navigate the healthcare system so much easier to simply send them down the hall for lab work and other important testing,” added Andrefsky. “I think it will reduce delays in care, and improve long term health outcomes for our patients.”
See photos from both grand opening events below.