In yet another monumental achievement made possible through the hard work of our One Amazing Team and your commitment to every child and family we serve, Texas Children’s has earned recognition from U.S. News & World Report as the #2 children’s hospital in the country.
In addition to Texas Children’s historic rise to #2 in the overall list, the 2022-23 U.S. News & World Report Best Children’s Hospital survey included Top 10 spots for every subspecialty:
- #1 in Cardiology & Heart Surgery, in a testament to the cutting-edge treatments and family-centered care provided by the Heart Center for more than 60 years
- #1 in Pulmonology
- #2 in Neurology & Neurosurgery
- #3 in Nephrology (kidney disorders)
- #3 in Neonatology
- #4 in Cancer
- #4 in Gastroenterology & GI Surgery
- #5 in Diabetes & Endocrinology
- #5 in Urology
- #8 in Orthopedics
Texas Children’s is also ranked as the #1 children’s hospital in Texas and #1 in the Southwest Region – rounding out the national honors in what President and CEO Mark A. Wallace called a “pivotal moment that reflected everything we’ve accomplished together this year.”
“These tremendous outcomes are the result of the steadfast leadership, unwavering dedication and sincere passion you have for Texas Children’s mission,” Wallace wrote in announcing the exciting news to the organization. “Our eight in-chiefs, our five executive vice presidents, our medical and administrative leaders, and our faculty and staff are without a doubt the greatest teams in our organization’s history.”
Reaching the top of the list
U.S. News & World Report introduced the Best Children’s Hospitals ranking in 2007 to help families of children with rare or life-threatening illnesses find the best medical care available. The rankings are the most comprehensive source of quality-related information on U.S. pediatric hospitals.
They rely on clinical data from nearly 200 medical centers through a detailed survey that analyzes measures, such as patient safety, infection prevention and adequacy of nurse staffing. In addition, each hospital’s score is derived from surveys of more than 15,000 pediatric specialists who are asked where they would send the sickest children in their specialty.
In 2021, only 89 children’s hospitals were ranked in at least one of the 10 pediatric specialties evaluated for the annual report. Ten hospitals ranked at the top of their class and were named to the 2022-2023 Honor Roll. For more information, visit usnews.com/childrenshospitals.
“Consistent collaboration, newfound discoveries and extraordinary patient care is what has brought us to where we are today. But we all know that for Texas Children’s, this is only the beginning of our bright future ahead,” Wallace said. “Let’s cherish and celebrate this moment – and then let’s gear up to climb even higher. I have no doubt that with this team, everything is possible!”
To read the full news release announcing Texas Children’s latest rankings from U.S. News & World Report, click here.



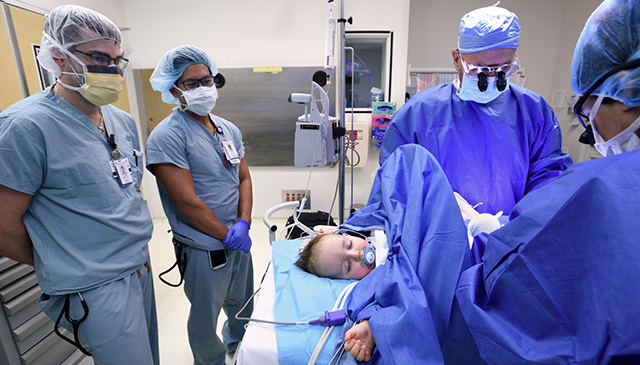
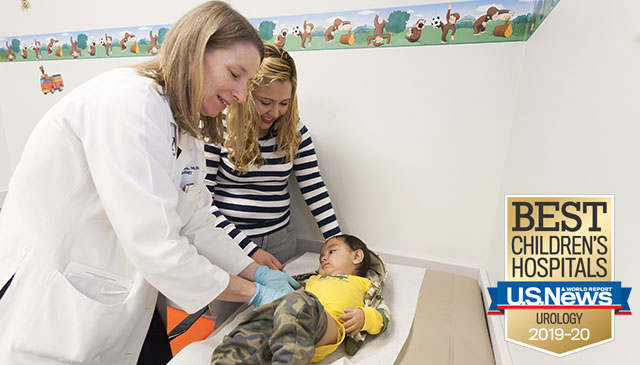







 The Southwest Pediatric Device Consortium (SWPDC), anchored at Texas Children’s Hospital and Baylor College of Medicine, recently received a prestigious P50 grant from the U.S. Food and Drug Administration. The five-year, $6.75 million grant will begin on September 1 and will allow SWPDC to leverage ongoing activities to expand and accelerate the development of much-needed pediatric medical devices. The five principal investigators include Drs. Chester Koh and Henri Justino of Texas Children’s and Baylor, Dr. Balakrishna Haridas of Texas A&M University, Dr. Maria Oden of Rice University, and Dr. Michael Heffernan of Fannin Innovation Studio.
The Southwest Pediatric Device Consortium (SWPDC), anchored at Texas Children’s Hospital and Baylor College of Medicine, recently received a prestigious P50 grant from the U.S. Food and Drug Administration. The five-year, $6.75 million grant will begin on September 1 and will allow SWPDC to leverage ongoing activities to expand and accelerate the development of much-needed pediatric medical devices. The five principal investigators include Drs. Chester Koh and Henri Justino of Texas Children’s and Baylor, Dr. Balakrishna Haridas of Texas A&M University, Dr. Maria Oden of Rice University, and Dr. Michael Heffernan of Fannin Innovation Studio.