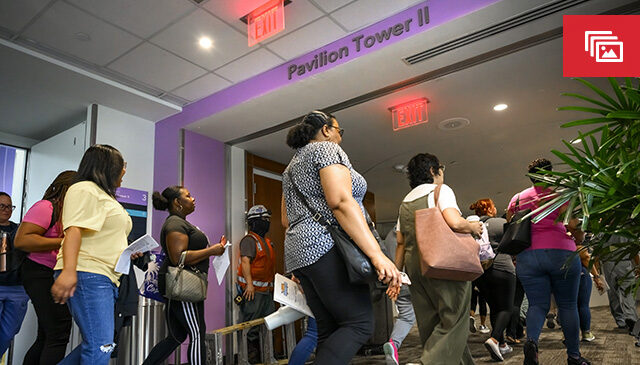
With the first phase of Texas Children’s Pavilion for Women’s $245 million expansion complete, outpatient OB/GYN practices recently moved to their new home across the street at Pavilion Tower II. The former Baylor Clinic building (located at 6620 Main Street) will transform into Texas Children’s newest medical tower upon completion – adding 190,000 square feet to the hospital’s footprint, improving patient access and creating space for more adult inpatient and neonatal intensive care beds within the Pavilion for Women.
“This investment in our Pavilion for Women will allow us to increase delivery volumes significantly, but additionally the added space will allow us to continue to grow these specialized clinics that cater to women at every stage of life,” said Michele Birsinger, assistant vice president of Women’s Services.
First to migrate was the Women’s Specialists of Houston (WSH) team on June 12, followed by Partners in OB/GYN Care (POGC) on July 18. Both groups halted clinic operations for moving day, gathering bright and early to ceremoniously turn the lights out in their old space and walk together to the new tower. Clinic leaders shared inspiring remarks upon arrival, and a workforce chaplain was present to facilitate a Blessing of the Hands and gratefulness prayer before lights were turned on with excitement and cheer.
We want to emphasize the importance of the people, read the moving day pamphlet. The Pavilion Tower II is a state-of-the-art facility, but without the people, processes and programs in place, it’s just a facility…the dedicated, intelligent and passionate faces that light up our clinics will remain the same for our patients and families.
To mark the special occasion, team members participated in a scavenger hunt to get familiar with their new floors and were treated to gift bags and mini Zen gardens for their desks. Workforce Well-being was also on hand to provide resources and gather insights on how to best equip and decorate respite rooms.
Before the OB/GYN clinics relocated, our Women’s Physical Therapy team were some of the first occupants of the new medical tower.
“Although we’ve offered physical therapy services since 2012, this is the first time we’ve had our own designated space,” said Sarah Ammons, specialty therapy coordinator. “We now have eight treatment rooms and a gym area, including cardiovascular and strength training equipment…care will improve greatly now that we have the space and resources to treat our patients more completely and return them to their prior level of function.”
These clinics are now open for patient activity – you can find WSH on Level 13 and POGC on Level 11 of the new medical tower, just follow the signs on the sky bridge on Level 3 of the Pavilion for Women. Baylor OB/GYN will relocate by the end of 2023, and the full Pavilion for Women expansion will complete in 2024.
Click here to read more on this exciting development.